In the behavioral science field, we spend a lot of time studying cognitive biases to understand their impact on how individuals make decisions and the actions they take. One cognitive bias that shows up in the context of health interactions is ingroup/outgroup bias: a pattern of favoring one’s own “ingroup” (a social group with which one identifies) over “outgroup” members (a social group with which one does not identify).
How to Leverage this Bias for Success
Ingroup/outgroup bias can contribute to positive behavior change when leveraged appropriately, but it can also interfere with those efforts if it’s ignored or misunderstood. When this bias presents itself in healthcare, health systems need to respond by mitigating potential negative impacts and using the bias to advance patient care. This starts with your patient communication and engagement strategies.
Here are a few ways to leverage ingroup/outgroup bias in the messages you share, for better patient outcomes overall.
1. Redefine Groups
In order to mitigate negative impacts and leverage ingroup/outgroup bias for good, you need to have an understanding of who your patients think they are – their self-identity. Additionally, you need to learn how they see themselves and their relationship with your health system. Who do they think they are and which groups do they identify with as a result? Who do they think you are, and do they view you as belonging to their same group(s)?
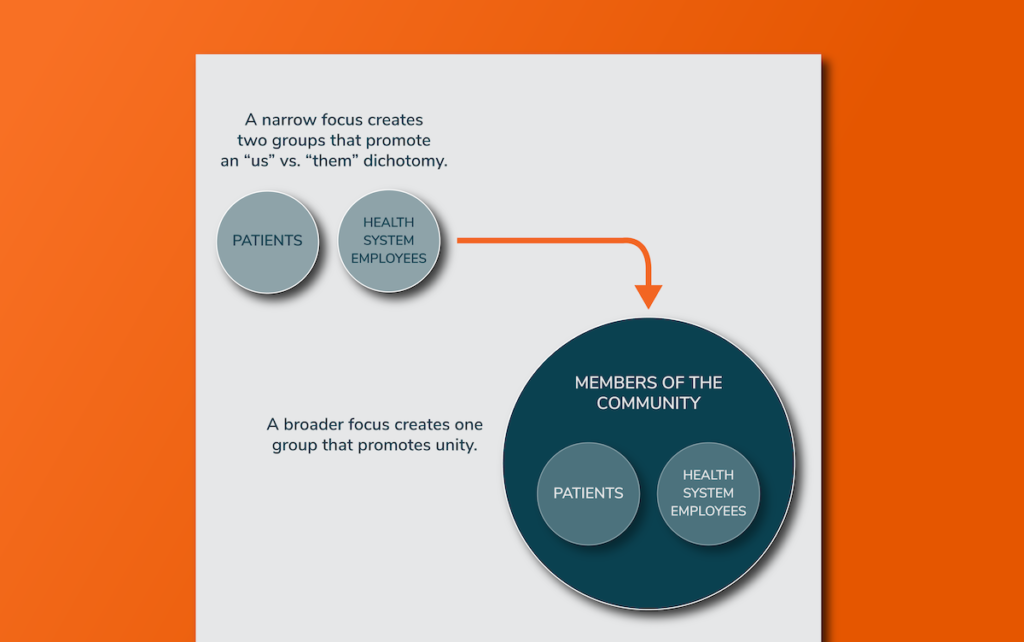
If patients view your health system and its employees as members of an outgroup, you have an opportunity to either redefine how patients sees themselves, change how patients see the health system, or both. You can do this by altering—usually expanding—the criteria used to define ingroups, and communicating messages with these new definitions. For example, defining parties as “patients” and the “health system” creates an “us” and “them” dichotomy—establishing two different groups with their inherent competition. However, defining all parties as “members of the community” establishes a single group to which everyone belongs. Highlight criteria you have in common to establish an ingroup that you both identify with.
This can include promoting affiliations and partnerships with local organizations that your patients are part of. For example, in a recent Lirio webinar, Dr. Deborah Stamps, Chief Diversity and Inclusion Officer and Executive Vice President of Quality, Safety, and Innovation at Rochester Regional Health, discussed the organization’s work with local churches that serve predominantly Black and LatinX communities, to provide information about the COVID-19 vaccine, given the virus’s disproportionately negative impact on racial and ethnic minorities. By aligning with these churches, the health system created a common point of interest with its patients and established membership in the same ingroup.
2. Promote Group Norms
Social groups have unwritten rules about how their members should behave. These are called “group norms” and represent the accepted standards of behavior for members of the group. Since people derive a portion of their self-identity from their membership in social groups, group norms exert significant influence over member behavior, creating a strong desire to conform.
Take advantage of this by positioning the desired behavior as normative for the group. For example, in your efforts to increase COVID-19 vaccine adoption, highlight membership in a group like “our local community” and reinforce vaccination as normative behavior for people who are members of that group. Your messages should make them think “I am a [city] resident, and [city] residents get vaccinated.” This appeal to ingroup bias counteracts vaccine hesitancy.
3. Employ Hyper-Personalized Messages
Health systems can strengthen the effectiveness of patient communication by making the messages hyper-personalized. This means allowing all patients to identify with and participate in all initiatives/programs relevant to them but reaching them via tailored approaches.
Hyper-personalized messages account for the recipients’ SDOH and potential cognitive biases and barriers at play. They overcome barriers, speak to the whole person and move them toward healthy behaviors and actions.
Move Patients toward Better Health with Lirio
Lirio’s behavior change AI platform helps health systems leverage behavioral science insights like the effects of ingroup/outgroup bias, by using Lirio Precision Nudging™ to develop hyper-personalized communication. We take the following steps to make this happen:
- Apply behavioral science knowledge to inform the problem the AI needs to solve. These problems center around moving patients to take specific actions for their health, like getting vaccinated or scheduling a preventive screening.
- Match behavioral science solutions with each patient based on what will be most effective in overcoming his or her individual biases and barriers.
- Deploy hyper-personalized messages at scale via continuous learning. Our machine learning agent gets smarter over time, makes adjustments to the messages, and allows you to reach more people across your patient populations.
Register for Our Next Webinar
If you want to learn more about how Lirio works with health systems to deliver hyper-personalized communication that drives improved outcomes, join us on Friday, June 18 for our next webinar, “Beyond Consumerism: Building Trusting Patient Relationships in the Digital Era.”
Our Chief Evangelist, Patrick Hunt, will speak with Sandra Mackey, Chief Marketing Officer at Bon Secours Mercy Health, about the changing role of the CMO and the importance of fostering patient experiences that are relational, rather than transactional.
Sign up today to save your spot.
Follow Lirio on Facebook: Facebook.com/lirio.llc, LinkedIn: LinkedIn.com/company/lirio, and Twitter: @Lirio_LLC.
Other readers viewed:
Lirio Launches Hyper-Personalized Vaccination Journey to Encourage Vaccine Acceptance
How to Make Patient-Centered Care Sustainable
How Behavior Change AI Addresses SDOH
How to Connect with Patients as Individuals: 10 Behavioral Biases Health Systems Should Know

